“When I was a bit younger, as a young teaching physician at the hospital, I found myself arguing with a homeless man. And despite the fact there was a snowstorm outside, he insisted on leaving against medical advice. I lost my argument with that man and I later learned that he had frozen to death. That man haunted me. Our hospital was supposed to be a place of healing, but he had chosen to face death rather than to accept our care. I began to wonder if maybe the sickest patient was actually the healthcare system itself… Never have we actually focused on the reality of our patients.”
~Dr. Jim Withers, founder of Operation Safety Net
So begins a riveting Tedx Talk about the Street Medicine movement that has countless healthcare workers taking the battle to the streets, providing diagnosis and treatment to some of America’s most vulnerable. (Check out this video interview between Invisible People’s Mark Horvath and Dr. Withers to learn more!) What motivates healthcare workers to volunteer their time and resources in this way? How effective is this initiative?
If You Want to Help People Heal, You Have to Go to Where They Are
If the Street Medicine philosophy was a tagline, that’s how it would read. Engaging vulnerable homeless where they are and on their own terms is vital. Why the urgency?
“Homelessness is hazardous to one’s health, and homelessness kills.” ~G. Robert Watts, CEO of National Health Care for the Homeless Council
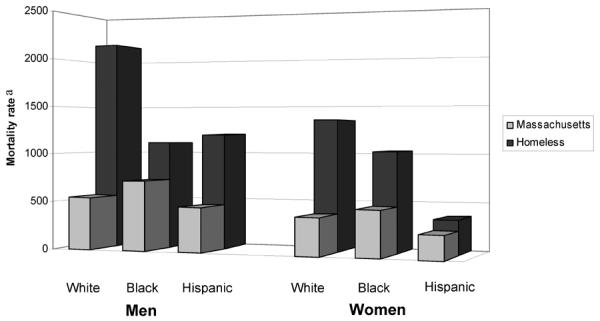
Mr. Watts isn’t wrong. Studies (here and here) conducted by Boston Health Care for the Homeless Program reveal that homeless people are four times more likely to die prematurely than their housed counterparts. This is often as a result of preventable and treatable chronic medical conditions. Why the increased mortality rates? The Association of American Medical Colleges explains “homeless people often have conditions that are aggravated by sporadic care and the rigors of their living situations, from chronic diseases such as diabetes to acute ailments, mental illness, or substance addiction.” Medical treatment is frequently sought only after a medical emergency occurs. Often, it’s a case of too little, too late.
And that’s where the Street Medicine movement kicks in.
Healthcare workers see themselves as offering a form of intermediate medical care. In every encounter, workers make efforts to identify and refer patients to a primary care facility as required. This strategy of taking the first step and going to where sick homeless people are living is an essential part of the process to build trust between client and healthcare provider.
An outreach program in Buffalo is aiming to build bridges between homeless individuals in that city and healthcare workers of the future. The University of Buffalo’s Jacobs School of Medicine and Biomedical Sciences sends students, faculty members and medical supplies to Buffalo’s central bus station. They conduct rounds on the streets and listen to homeless patients’ symptoms to get a picture of their healthcare needs. Then the medical team creates a comprehensive treatment strategy.
Thea James, vice president of a similar medical school program run out of Boston Medical Center, identifies why unsheltered individuals are particularly vulnerable to deteriorating health. “In medical school, we are taught to focus on treatment of the medical problems patients present with. But as a provider, you have to find out what is driving disease instability to break the cycle. When a person doesn’t have secure housing, that becomes a driver of health instability.”
Healthcare on the Mend?
Medical needs within the homeless community require more than a band aid solution. However, we are seeing encouraging results.
Let’s go back to the work being done by Boston Health Care for the Homeless Program, which treats over 10,000 homeless adults and children. One study showed efforts cured 97% of patients treated for hepatitis C. BHCHP also treated 259 patients with HIV during the 2016-2017 calendar years, of whom 92% received HIV medications and 89% reached undetectable viral loads.
Less data driven, but perhaps more important are the relationships healthcare workers build with vulnerable homeless people. One man who was treated on the street made this telling statement: “I can’t believe someone cares that we’re still alive!”
James O’Connell, president of BHCHP, is realistic about the benefits and limits of Street Medicine initiatives. “Even though we can’t solve their homelessness, we can ease suffering and treat potentially deadly diseases,” he said.
Joel Hunt, who works at a homeless encampment near Fort Worth, Texas, puts it this way: “[Homeless people are] not talked about in a fond, kind of normal, humanizing way. Having somebody check in on them because they’re human goes a long way to adding dignity, adding hope.”
Dr. Jim Withers, quoted at the outset, concluded his Tedx Talk with a story and a challenge:
“Ultimately, it’s about human connection. Two months ago, a dear friend of mine on the street was tragically burned. In fact, his leg had to be amputated. I went to visit him and as he lay in his hospital bed. I asked him, ‘Do you have any family?’ I’ll never forget a tear coming down his cheek and he looked at me and said, ‘You people are my family!’ That kind of connection is powerful, sacred stuff. And I knew that whatever happened we would be in this together, and that felt really good.
“Do we have the courage to move into the reality of our brothers and sisters? I believe ultimately we have to, because as I tell my street friends, we’re all in this together.”